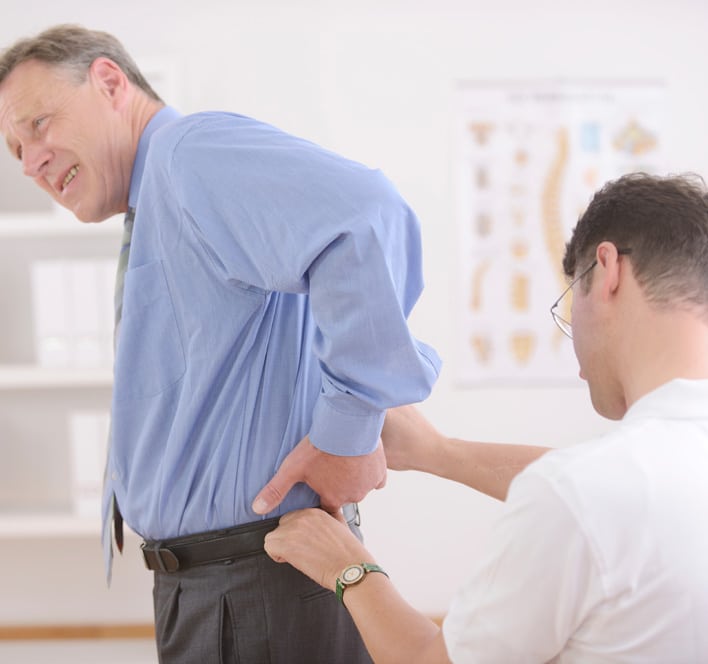
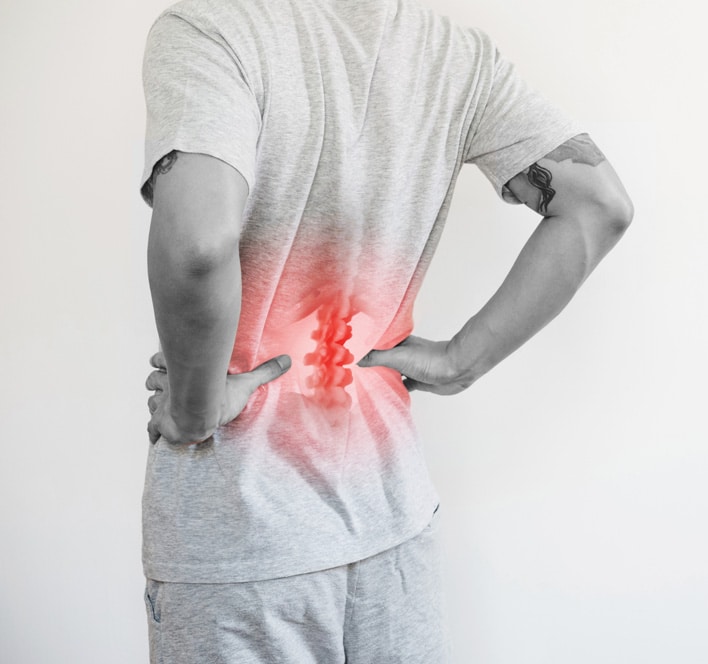
Interlaminar Spacer Recovery Timeline: What to Expect During Each Phase
Undergoing surgery can be a daunting process, and the recovery that follows is often just as concerning. For those who have received an interlaminar spacer, understanding what to expect during recovery can help ease anxiety and set realistic expectations. The recovery process is usually broken down into distinct phases, each with its own goals and ...