The spinal column has several components working together to ensure that your neck and back function properly. It serves a vital role in your body’s protection and functioning. A healthy spinal column allows you to stretch, bend, lean, and rotate. It also helps you maintain your balance and posture while protecting the spinal cord.
Problems with the spinal column can lead to pain, muscle weakness, and decreased range of motion. This is especially true for the discs in between each vertebra. Injury, degenerative disc disease, and everyday wear and tear cause damage to the discs. In some cases, the pain can be a nuisance. Other times it severely limits your day-to-day functioning.
Disc pain is usually associated with the lower back or neck area. These areas of the spine have the most mobility. The increased movement, along with the challenging task of supporting the body, often wears away at the intervertebral discs.
Let’s take a look at the intervertebral discs and the common problems with them that can lead to pain.
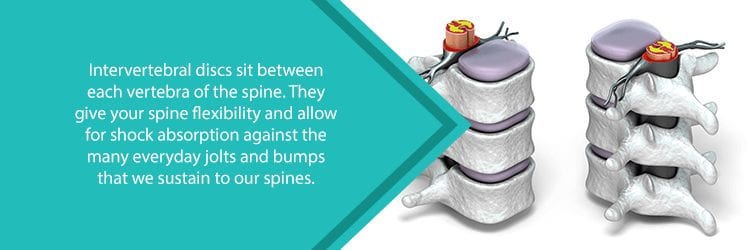
What is an Intervertebral Disc?
In between each vertebrate is a round ligament, known as a disc, that keeps these bones connected. Discs provide the spine with shock absorption during the body’s everyday movements. In addition, discs give the spine added stability and allow for movement.
Each disc is made of two main parts:
- Annulus Fibrosus: The outer layer of the disc is composed of strong ligament fibers. It connects the vertebrae and distributes pressure evenly throughout the disc. It also protects the inner layer from leaking out of the disc.
- Nucleus Pulposus: The inner layer of the disc is a jelly-like structure composed of water and collagen fibers. This flexible area provides shock absorption and protects the spinal cord and nerve roots.
Lower back and neck pain can be caused by damage to either layer of the disc.
The ABCs of Disc Pain
Disc pain occurs for a variety of reasons. Here are common conditions:
A: Annular Tears
Ligaments are flexible, fibrous tissues that connect our bones and hold together the joints. Like your elbow, knee, and ankle, your discs are prone to injury. When the outer layer of the disc tears or ruptures, this is known as an annular tear.
In many cases, annular tears are due to the body’s natural aging process. As we grow older, our discs start to break down, losing their strength and flexibility. This is known as degenerative disc disease. In fact, even in our thirties, our discs start to show signs of wear and tear.
The slow breakdown of our discs puts them at risk for annular tears. Repetitive movements, high impact activities, or sitting for long periods make the discs more prone to annular tears. Car accidents and sports injuries are also a common cause for this type of injury. Most tears start from inside the annulus fibrosus and extend outward.
Minor annular tears often don’t have any symptoms. If the damage is more severe, you may experience pain in the back or neck while moving or sitting for long periods. Untreated annular tears could lead to more severe conditions like bulging discs.

B: Bulging Discs
The natural aging process causes the discs to dehydrate and lose their original form. In some cases, this causes the discs to bulge. This occurs when the larger part of the disc spreads beyond its normal boundaries. For many, this common disc condition doesn’t show any symptoms. Many people don’t even realize they have bulging discs. If the bulge extends enough to affect a nearby nerve, symptoms usually occur.
Most people experience bulging discs in the lower back. When a bulging disc causes a pinched nerve, you may experience pain that radiates from the back to the buttocks, legs, and feet. For bulging discs in the neck, the pain can spread from the neck all the way to the fingers.
A herniated disc is another abnormality that can occur in the disc. It results when the disc’s outer layer cracks and the soft inner layer protrudes outside the disc’s perimeter. A herniated disc can affect surrounding nerves and cause pain or other issues. This is due to the compression of nerves or the inflammation of nerve roots.
Pain symptoms are similar to a severely bulging disc. The added pressure on the nerve can also cause numbness and tingling. As the nerve weakens, you may experience muscle weakness. This impairs your ability to walk or lift and hold items.
C: Collapsed Discs
A collapsed disc occurs when the outer disc layer deteriorates enough that it loses shape. Like the previous conditions, it can occur because of the normal aging process as well as traumatic injury. During our daily activities, the inner layer of our discs presses against the outer layer. Eventually, the outer layer loses its elasticity and can no longer maintain the height and shape of the disc.
Symptoms of a collapsed disc occur when there is compression on the nerve roots or spinal cord. These symptoms vary based on the severity of neural compression. You may experience pain in the back, neck, and extremities. In addition, tingling and numbness are common along the path of the affected nerve. In more severe cases, muscle spasms, weakness, or loss of functioning can occur because of the damaged nerve.

Treatments for Disc Pain
As mentioned earlier, some people with these conditions experience little to no pain. Others experience symptoms when the disc compresses surrounding nerves or the spinal cord.
When the symptoms of disc pain affect your everyday life, you may wish to consult with a physician for a full medical exam and diagnostic imaging. An accurate diagnosis allows your physician to determine the most appropriate care. Some disc problems only require conservative treatment. Others may need minimally invasive spine surgery.
Here are some common treatment options for disc pain:
Rest
Rest is certainly the cheapest, easiest treatment option for minor disc pain. Resting the area gives it time to reduce swelling. Try to avoid activities like sports, heavy lifting, or bending if you’re experiencing neck or back pain.
While resting the area, you may be advised to use ice and/or heat to relieve pain. This approach can help minor instances of inflammation, but damaged discs may require additional treatment.
Pain Medication
Over-the-counter pain medications may help reduce swelling and pain. If pain persists for more than ten days, however, you will want to consult with your doctor.
Doctors or pain specialists can use a variety of prescription pain medications to treat pain. If the pain is severe, you may be prescribed narcotics like codeine or oxycodone-acetaminophen. Though these medications effectively relieve pain, they could be habit-forming—especially for someone who has a history of addiction. You should always weigh the risks and rewards of each prescribed medication.
If you have nerve damage, a doctor may also prescribe certain medications like amitriptyline or gabapentin. Muscle relaxants can also help with muscle spasm and tightness.
Steroid injections bring anti-inflammatory medications directly to the source of pain. Injections can be used if you’re not responding to oral medications.

Physical Therapy
In some cases, physical therapy is a great alternative to dangerous prescription pain medications. A physical therapist works with you to strengthen and increase flexibility in muscles affected by a damaged disc. They provide specific activities to help restore movement and reduce pain.
Physical therapists also educate you on your condition, the habits you need to change, and strategies to improve your overall functioning.
Minimally Invasive Spine Surgery
While conservative treatments often help a person feel better, sometimes a disc is so damaged surgery is necessary. Luckily, medical advances have made damaged disc surgery safer and more effective than ever.
If your discomfort isn’t relieved by conservative treatments or gets worse, surgery might be the best option. Surgery can include:
- Microdiscectomy: This minimally invasive procedure removes a portion of the damaged disc to take pressure off the affected nerve. The area is stabilized to prevent further nerve compression.
- Artificial Disc Replacement: During this procedure, the entire damaged disc is removed. A prosthetic implant is inserted to assist the spine in maintaining motion.
- Spinal Fusion: This traditional approach involves removing the disc and replacing it with a bone graft. The surgeon stabilizes the area and eventually the two vertebrae that surround the damaged disc fuse together as one.
Don’t Delay Seeking Treatment
If your neck or back pain is keeping you from living the life you desire, NJ Spine & Orthopedic is ready to help. Our dedicated team will listen to your questions and concerns as well as review any previous MRIs. We empower you with the best information and options so you can decide which treatment is right for you.
NJ Spine & Orthopedic specializes in minimally invasive procedures designed to help get your life back. Don’t waste another day wondering how you will get relief. Schedule a consultation and see how we can help you get back to enjoying the activities you love.

