Your Ultra-Stable Thoracic Spine
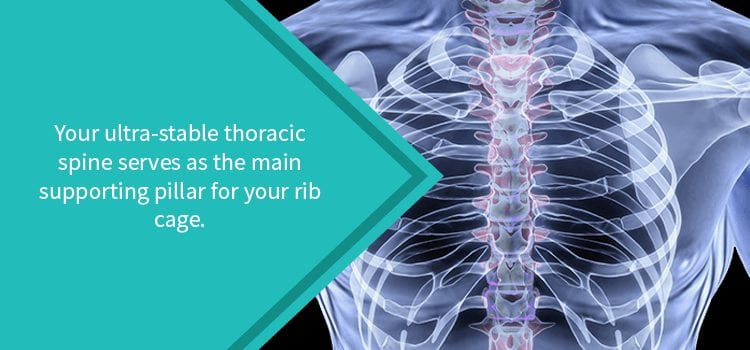
Your thoracic spine consists of 12 vertebrae, which extend from the base of your neck to the beginning of your lower back. While your cervical and lumbar spine segments enable movement and flexibility, your thoracic spine offers stability. Correspondingly, this ultra-stable design enables your thoracic spine to serve as the main supportive pillar for your rib cage.
In fact, each of your ribs sprouts from one of these thoracic vertebrae. Your ribs then arch around to the front of your body where they meet at your sternum. This strong cage formed by your ribs makes your thoracic spine more static, stable, reinforced, and less prone to injury. This does not, however, mean that your thoracic spine is incapable of sustaining an injury or generating pain.
There’s also a hidden downside to this stability: Your rigid thoracic spine contains less built-in spaces than other spinal segments. This translates to smaller intervertebral discs for shock absorption, less wiggle room between vertebrae, and a narrower spinal canal. And, with less wiggle room naturally comes increased chances for injuries, damage, and discomfort. A leading cause of this discomfort? Thoracic disc herniations.
Why Do Thoracic Disc Herniations Occur?
In essence, our intervertebral discs serve as shock-absorbing cushions between each vertebra in our spine. These rubbery discs absorb forces from bodily activity and permit smooth movement of the vertebrae as we navigate our day. Structured like a jelly donut, our spinal discs consist of a tough exterior filled with a viscous jelly-like interior.
With less space existing between each thoracic vertebra, our thoracic discs compensate by adopting a thinner design. Under normal circumstances, our thoracic discs do not need to absorb as much shock from spinal movement as do other spinal segments. However, as a result, these discs possess less lubricating and cushioning properties. Combined, these two factors can result in damage to thoracic discs. Often this occurs in the form of thoracic disc herniations.
A herniation occurs when the exterior of an intervertebral disc cracks open, expelling the gelatinous contents of the disc. This material can protrude into adjacent nerves, resulting in anywhere from a slight ache to excruciating pain. The smaller canal of the thoracic spine also leaves the spinal cord susceptible to the entrapment (sequestering) of herniated disc material.
Additional Risk Factors
A number of conditions and events can lead to thoracic disc herniation. However, the two most common triggering events include degenerative disc disease and traumatic injury. A particularly common condition, degenerative disc disease usually results from the aging process, as the effects of wear and tear accumulate on the spine.
Unfortunately for many, disc degeneration is virtually impossible to avoid. Especially, when we take into consideration the sheer number of workers who earn a living from careers that place chronic strain on the back. Nurses, construction workers, and athletes… All of these workers rely on their back for their wages.

In addition, sudden, traumatic injuries to the back can also lead to thoracic disc herniations. Car accidents… falls… even the occasional awkward movement can place undue strain on the thoracic spine, leading to disc rupture.
Symptoms of Thoracic Disc Herniation
As with disc herniations that affect other parts of the spine, symptoms of thoracic disc herniation can vary widely. Some cases will go unnoticed; some will cause minor pain; and others will cause debilitating side effects. Possible symptoms to look out for include:
- Back Pain: You will likely feel localized pain of varying intensities in your middle back.
- Pain associated with certain movements: Furthermore, pain may also intensify during certain movements and then subside during others. In particular, lying down may trigger pain, possibly leading to psychological symptoms such as insomnia or anxiety.
- Radiating pain down the legs: If your herniated disc causes radiculopathy (or pinched nerves), pain can migrate from the middle back into the legs.
- Abdominal Pain: Because the thoracic vertebrae connect to your ribs, you may experience a band of pain around the abdomen.
- Muscle Weakness: As a result of pinched nerves, surrounding muscles can become weak or stiff.
- Numbness: Localized or radiating numbness or tingling down the legs can also occur.

Treatments for Thoracic Disc Herniation
Treatments for thoracic disc herniations can vary just as widely as their symptoms. For some, observation & monitoring may be enough. (Minor disc herniations tend to improve and heal on their own.) If you choose to take this approach, your doctor will likely recommend rest, immobilization, & ice/heat application.
For those with mild to moderate pain associated with herniation, your doctor will likely prescribe medication. Nonsteroidal, anti-inflammatory NSAIDs work for many, whereas others will require prescription-strength options. Corticosteroid injections provide an additional option for localized, yet short-term, pain relief.
For those with more debilitating conditions, your physician may recommend surgery followed by a course of physical therapy. With a variety of minimally invasive options to address your condition, surgery can provide long-term relief from symptoms with less undesirable side effects than traditional, open back procedures. If you are suffering from a painful thoracic disc herniation, contact an orthopedic spine surgeon who can evaluate your best treatment options.

