Branching down the path that leads between your lower back and into each leg exists the sciatic nerve. If you experience pain that radiates along this area, then you may have a condition known as sciatica. In most cases, these symptoms are only felt on one side of the body (a symptom known as unilateral pain).
Often, other conditions like herniated discs, bone spurs, or spinal stenosis lead to sciatic nerve compression. These ailments are related to sciatica because each condition can result in the abnormal application of pressure to various points along the sciatic nerve. The common thread between cases of sciatica is that patients experience similar symptoms, like pain, inflammation, and numbness. Sometimes, this pain is quite severe. But, luckily, most cases of sciatica can be resolved with nonsurgical treatments. In more serious cases that involve significant weakness or loss of bladder/bowel control, the patient may need surgery.
Sciatica Resources
The Sciatic Nerve
Throughout the entire body, there is not a single nerve larger than the sciatic nerve. This structure is the product of individual nerve roots that branch out from the lower spine. In cases of sciatica, this structure becomes irritated when pressure is applied to a point near the beginning of the nerve.
More specifically, the sciatic nerve starts at segment L3, which extends from the lower back. In fact, at every level of the lumbar spine, nerve roots exit from the canal’s internal cavity. Outside of the spinal canal, these nerve roots weave together into the structure known as the sciatic nerve. The nerve then runs down through the buttocks and the anterior side of each leg. Additionally, the sciatic nerve branches out at different points along its path, innervating different parts of the leg. This includes the thigh, calf, foot, and toes.
Because this is such a large nerve, there are many different locations from which sciatica may originate. These locations play a determining factor in the exact nature of the symptoms that will be experienced by patients.

Common Types of Sciatic Pain
When a patient is experiencing pain associated with sciatica, a doctor is usually able to trace the irritation point from the nature of the symptoms. The most sciatica pain symptoms include:
- Pain/numbness in the lower leg and foot: Sciatica of the L3-L4 level is usually the culprit of these discomforts. Additionally, it is not uncommon for patients to experience muscular weakness. Some patients may also find that they are not able to extend their foot upward. In other cases, patients with this form of sciatica will have a diminished knee-jerk reflex.
- Weakness in the extension of the big toe and ankle: This form of sciatica occurs in the L4-L5 segment. Sometimes, doctors refer to these symptoms as foot drop (weakening of muscles that flex the ankle and toes). Patients with this form of the disorder may also feel pain/numbness in the top of the foot. This is especially true between the big and second toes.
- Pain/numbness in the outer side of the foot: Patients with these symptoms have sciatica at the L5-S1 level. In addition to this pain, patients may experience muscle weakness in this area of the lower back as well. In fact, sciatica and lower back pain go hand-in-hand. This weakness also leads to difficulty with raising the heel off the ground, resulting in the patient walking on their tiptoes. In some cases, patients with this form of sciatica have a diminished ankle-jerk reflex.
It is important to remember that these symptoms are simply the most common and not the only possible symptoms of this condition. Problems arising from sciatica differ across numerous variables, ranging from individual anatomy to specific pathology.
Common Causes of Sciatic Nerve Compression
As mentioned previously, pre-existing conditions within the spine often cause sciatica. Herniated discs are the most common cause of sciatica-associated pain. Other sciatica causes include:
- Spondylolisthesis (aka a slipped vertebra)
- Lumbar degenerative disc disease
- Spinal stenosis (aka narrowing of the spinal canal)
- Spinal arthritis
- Bone spurs
It should be noted that while sciatica-associated symptoms are often caused by lumbar spine anomalies, there are other conditions that are very similar:
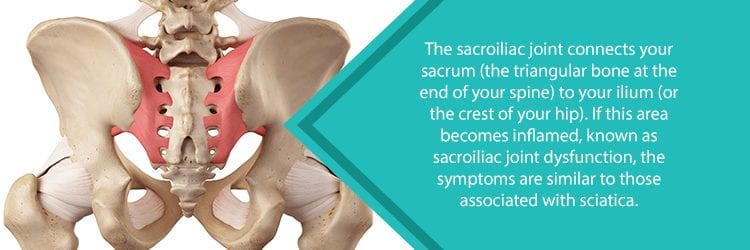
- Sacroiliac Joint Dysfunction: Patients with this dysfunction experience very similar symptoms to those associated with sciatica. This condition gives patients a deep, aching pain felt inside the leg. This differs slightly from the pain associated with sciatica, as it is not as well-defined or linear.
- Piriformis Syndrome: This condition occurs when a muscle located within the buttocks (specifically, the piriformis) spasms, leading to pain and discomfort. Because of its close proximity, this may also irritate the sciatic nerve, causing a type of pain very similar to that of sciatica. However, usually, the pain is much more intense above the knee than it is with sciatica. Additionally, the point of origin for the pain often originates in the buttocks as opposed to the lower back. In fact, piriformis syndrome does not usually affect the lower back at all.
Risk Factors for Sciatica
The presence of any of the following risk factors may also increase the likelihood that sciatica will develop:
- Obesity: Excess body weight may put additional pressure on the spine. This pressure leads to spinal anomalies that commonly cause this condition.
- Prolonged Sitting: Active people are much less likely to develop sciatica than those with a more sedentary lifestyle.
- Diabetes: Not only does this condition affect how your body processes sugar, but it also increases your chances of sustaining nerve damage.
- Age: One of the most common reasons that people develop sciatica. As we age, our bodies become more prone to developing all kinds of medical conditions, such as bone spurs and herniated discs. Spine conditions such as these often lead to sciatica.
- Occupation: One of the most common causes for back injury is improper lifting technique. Jobs that require heaving lifting, twisting, or driving for long periods increase the incidence of sciatica.

Treatments for Sciatica
Sciatica pain relief may be achieved through both surgical and nonsurgical methods. Whether or not treatment is necessary depends entirely on the persistence and severity of sciatic episodes.
Nonsurgical & Conservative Treatments
Simply put, there are numerous conservative treatment options for people who suffer from sciatica. Some of the most common examples are:
- Heat/Ice: For more isolated and less severe instances of pain, heat/ice pack application helps to remedy pain and discomfort. It is best to apply this method in 20-minute increments, every two hours. Whether or not you decide to use heat or ice is entirely up to your preference, so you should experiment with both. If you decide to use ice, make sure to protect your skin with a towel or cloth to avoid skin irritation.
- Pain Medications: Over-the-counter and prescription medications may help to alleviate the pain associated with sciatica. More specifically, oral steroids or NSAIDs can reduce inflammation and muscle relaxants work to relieve aches and spasms. Narcotic medications may also help with pain relief in cases where muscle relaxants do not work. In more severe cases, however, your doctor may prescribe epidural steroid injections. This solution, however, is often temporary and must be repeated about every 6 months.
- Physical Therapy: It is best to do your research or consult a therapist for advice on the best pain-relieving exercises. Cautious experimentation with strengthening, stretching, and low-impact aerobic exercise will help you find what works best for you.
Minimally Invasive Surgical Treatments
Doctors usually consider surgery for sciatica only in severe cases where there is progressive weakness or the appearance cauda equina syndrome (a debilitating condition that can lead to permanent paralysis). Depending on your case, your doctor will likely suggest one of the following surgical methods to address your condition:
- Microdiscectomy: This is the most common approach, usually reserved for cases in which a herniated disc is impinging on a nerve. Using tiny instruments and magnification, a doctor removes the portion of the abnormal disc that is causing the pinched nerve.
- Lumbar Laminectomy: A surgeon may recommend this approach for sciatica cases that are caused by lumbar spinal stenosis. For this procedure, the performing doctor partially removes the bone or disc material that is putting pressure on the nerve root.
Do you have recurring episodes of pain that aren’t getting better with time?
If so, please contact NJ Spine and Ortho at (855) 586-2615. Our team of board-certified and experienced specialists is well-versed in the latest and greatest minimally invasive techniques. You can rest assured knowing that our team will create a personalized care plan tailored to suit your specific needs.
Frequently Asked Questions
Will sciatica get worse without treatment?
If the sciatic nerve is damaged, it could result in numbness, tingling and weakness in your lower extremities in the most severe cases. The longer sciatica is left untreated, the more difficult it will be to successfully treat the condition, potentially becoming permanent.
How long will it take my sciatica to go away?
For the majority of patients, acute sciatica pain resolves within a couple of weeks. However, certain patients may develop chronic sciatica pain which may increase and decrease, but remains present over many years. If you have recurring episodes of pain that aren’t getting better with time, contact NJSO to get started with a custom-tailored treatment plan.
Once sciatica goes away, will it come back?
Sciatica can and does come back, especially when a person has a chronic medical condition. People who do not make lifestyle changes to prevent more sciatic pain may also redevelop symptoms. If you have recurring episodes of pain that aren’t getting better with time, contact our board-certified and experienced specialists today to ensure your sciatica is properly treated for long-term relief.